
Going digital for Q15s and safety checks?
Three pillars for successful adoption: User Experience, Data, Equipment

Digital Q15s
For 20+ years, healthcare systems have been focused on going ‘paperless’ through the adoption of EHR/EMR/eMAR’s and more. Going paperless unlocks many benefits for health systems by increasing efficiency, transparency, and portability. In 2009, medical hospitals were incentivized though large subsidies to transition to EHR systems (CMS). However, psychiatric hospitals and other care centers were ineligible to receive this incentive (Health Affairs), and many behavioral health programs are only now catching up.
In this post, we focus on one behavioral health process that is still broadly paper-based and in need of an update: the safety check. These checks are the Q15s, 1-on-1s, Q30s, Q60s, safety checks, and environmental checks that are conducted by front-line health techs in psychiatric hospitals and residential treatment facilities across the country.
If You’re Going Digital…
Even for a seemingly straightforward process like safety checks, there are a number of factors to assess before transitioning away from paper.
First, there is the digital safety check tool itself. It needs to be at least as easy as your current system for your entire team: frontline staff, nurses, managers, records office, etc. If the system is more difficult or complex than using paper for anyone on the team, transitioning will feel like a burden and result in resistance and perhaps even failure of the transition.
Second, there must be great reporting capabilities. Moving from a paper system, where a manager might glance at Q15 forms, to a real-time digital system where there is a constant stream of data, requires careful data processing, visualization, and analytics.
Third, and possibly most importantly, there needs to be a solid infrastructure plan in place. This covers things like 24/7 connectivity, device procurement, device management, GPS & access tracking, and disaster contingency and recovery plans..
User Experience
As the first step of going digital - the app needs to be great. And ‘great’ should not be confused with ‘lots of features’. We’ve all seen a bloated EHR, right?
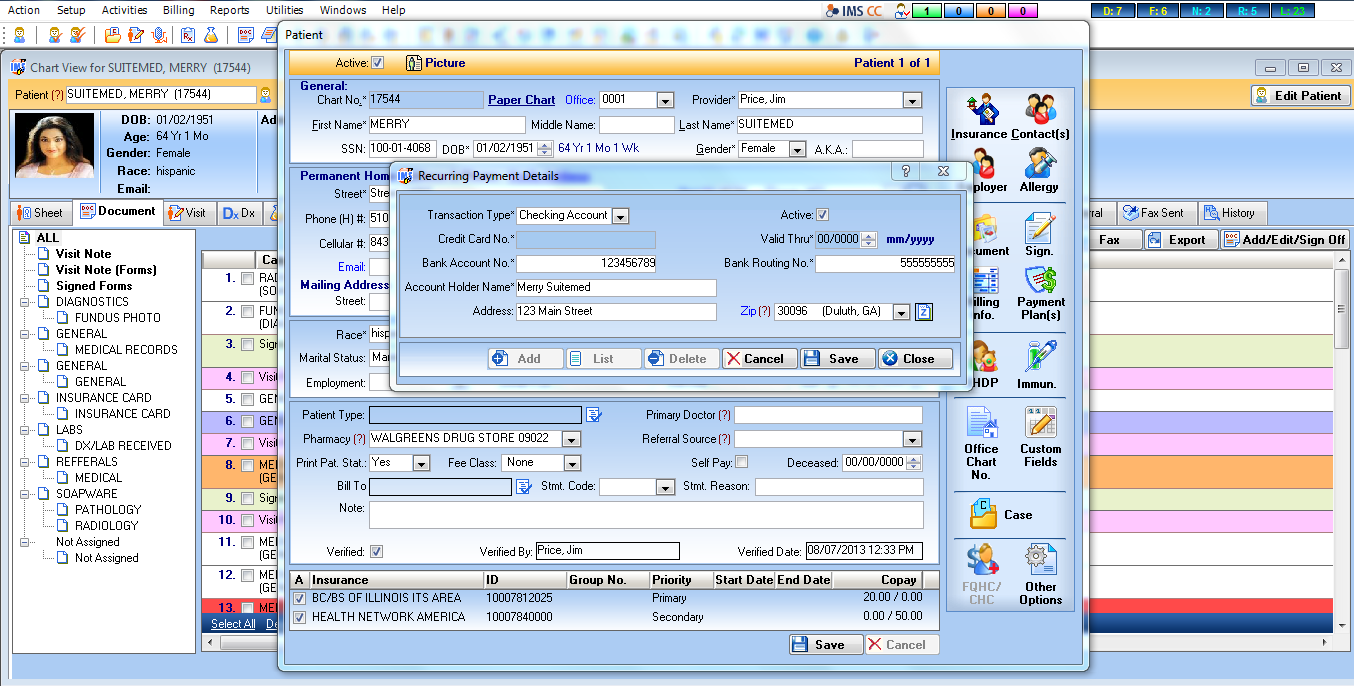
Another bloated EHR workflow
‘Great’, in the context of a digital Q15 app, is about simplicity. It is easy to add feature after feature to an application, but each feature has a cost in terms of ease-of-use, intuitiveness, speed, and even broader ripple effects like training costs.
The ‘gold standard’ is that the app must be easier and more intuitive than using the current paper system. Ideally, it would take no more than a minute for a user to be fully trained and comfortable with a digital Q15 app. This standard applies foremost to the health techs and front-line staff who will be conducting thousands of Q15s per day. But it also applies to nurses, who will use the app to conduct their nurse rounds, and managers, who track team accountability & compliance.
If any feature requires hands-on training, that effort must be multiplied across your entire team, today and in the future. Simplicity pays dividends in both the short and long term.
The Data
Once you have a great & simple safety check app in place, you will be introduced to a new constant stream of data. So much data that, if not processed simply and efficiently, the unit manager or program director might be quickly overwhelmed. Each safety check will contain information like; time of day, patient name, staff name, whether the check was on-time or late, patient location, patient activity, and even staff-to-patient proximity.
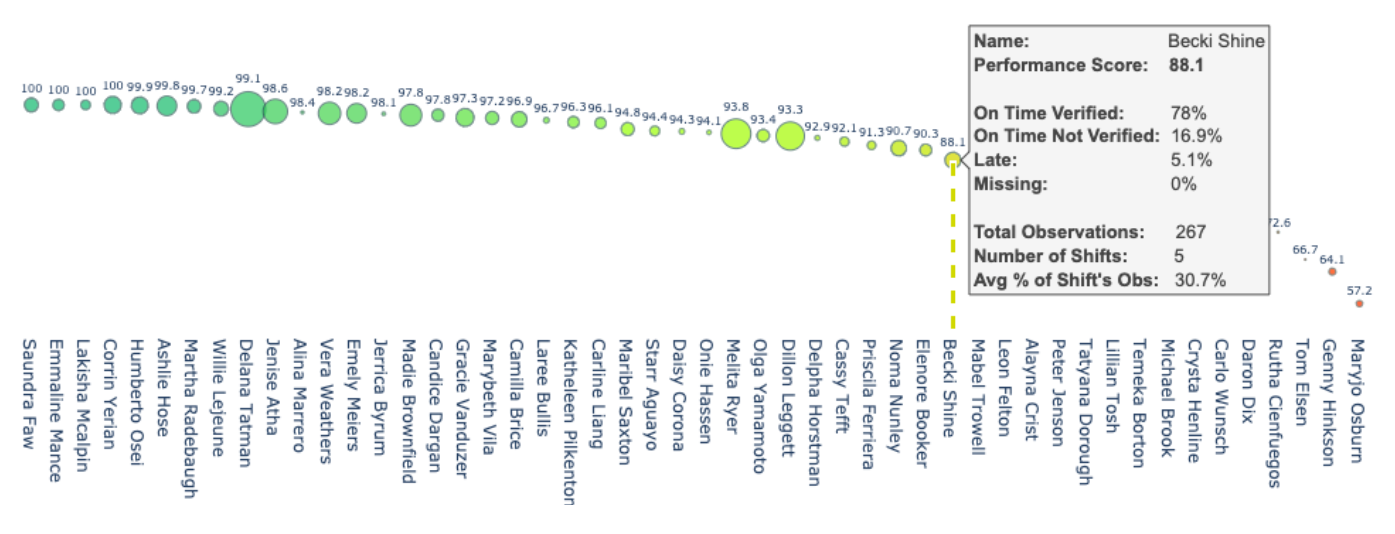
At-a-glance staff performance.
Safety dashboard, reports, analytics, and alerts need to work together in a way that improves transparency and accountability while reducing the time needed for managers to oversee compliance. It should be easy to see how individual staff members perform and easy to identify the role models and those in need of focused attention and training. Managers should be able to quickly see unit performance over time and executives should be able to monitor facility-level performance. Of course, the system must also generate the required reports for accrediting bodies (e.g. Joint Commission) and state surveyors.
Where simplicity is the cornerstone of a great Q15 app, intuitive reports and analytics are what will make or break the adoption of a digital rounding system for management teams.
The Equipment
The third and final pillar of successful digital safety check adoption is infrastructure and I.T. Device procurement, device management, data security, and 24/7 connectivity are table stakes. While device and data management can’t ensure successful adoption, a shortcoming in any of these areas can ensure failure. Some of the best laid tech adoption plans have been derailed by poor WiFi connectivity, unexpected equipment expenses, or seemingly trivial “back-end” issues.
For digital rounding/Q15 systems, the main elements are:
-
Device Selection & Procurement
-
Device Security & Management
-
Device Connectivity
-
Proximity Equipment - Management & Costs
-
Device Selection & Procurement
Once you have selected the quantity of devices needed (we recommend 1 handheld device per ~5 patient beds) you will need to select a device and supplier. Without exception, we recommend handheld mobile devices over tablets for ease of use and the ability for your team to quickly pocket the device they need their hands free. We also include accessories like cases and charging stations in this category.
- Device Security & Management
With devices selected, they now need to be locked down to restrict access to call/sms, unrestricted apps, camera, etc. This can be accomplished via an MDM vendor (mobile device management) or via an in-house I.T. team. The devices should be GPS-tracked and, ideally, geofenced so that your team can be alerted if they leave your campus. It should also be ensured that any system you use encrypts all data in transit and at rest, ideally with no local storage of protected health information (PHI) on the devices.
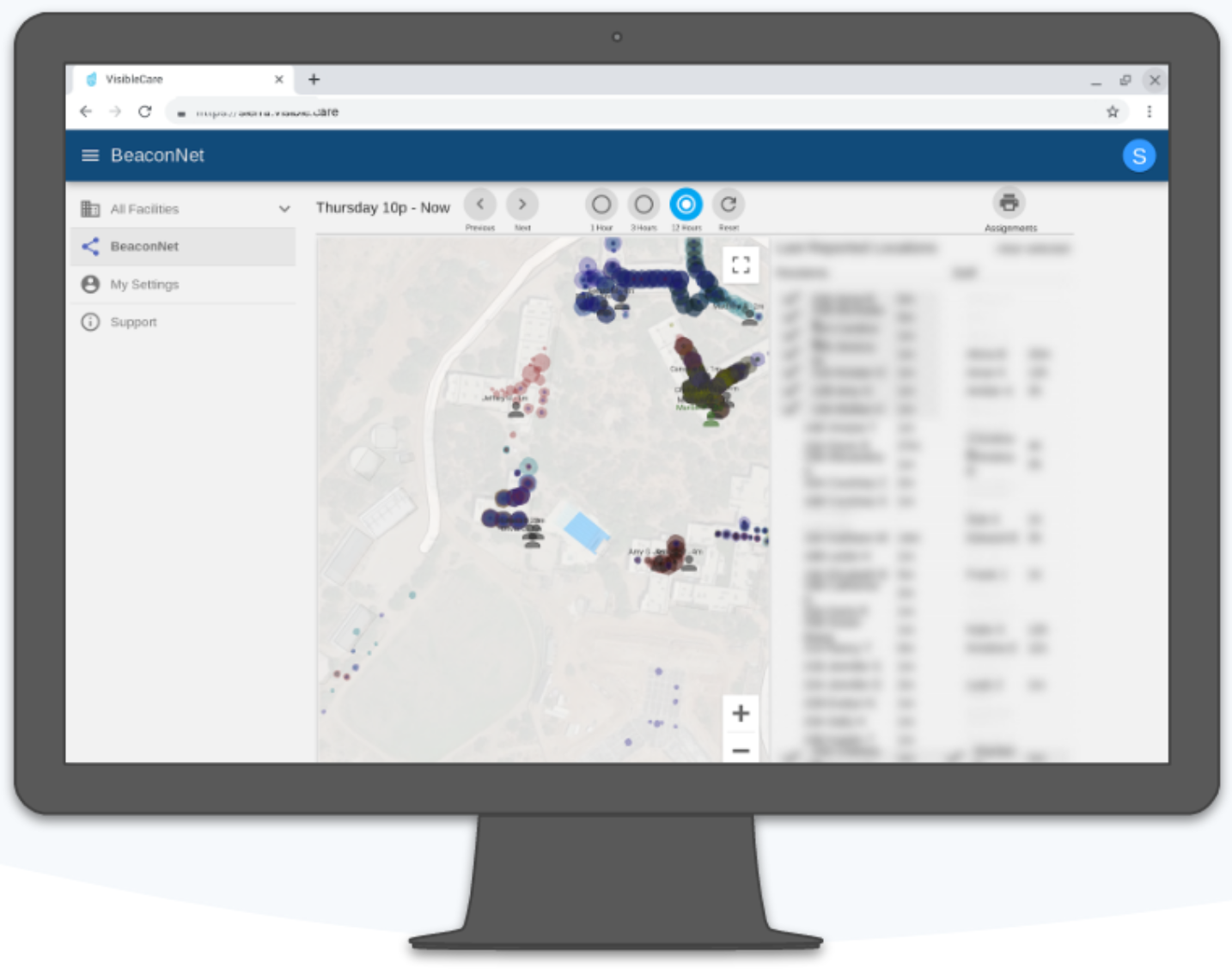
- Device Connectivity
Healthcare facilities are notorious for poor WiFi connectivity, and solid connectivity is essential for mission-critical applications like safety check Q15s. We recommend using cellular data for first-line connectivity, with local WiFi as a backup if needed. Rarely, if ever, have we seen local WiFi coverage that is more reliable than cellular. Some units/facilities may have cellular dead-spots, which should be managed gracefully by an ‘offline-mode’ in the safety rounding app. In addition to ensuring better coverage and up-time, cellular also gives programs the flexibility to move phones between units/buildings or off campus without management burden or connectivity outages.
- Proximity Equipment
For programs electing to use a Q15 safety check system with “proximity verification” there will be an added procurement, management and tracking process for whatever hardware is needed -- usually wristbands and beacons.. Per-band and per-beacon expenses are variable and tend to add up quickly for facilities doing hundreds of admits per month. When assessing products, be sure to investigate the expected ongoing costs of proximity equipment, expected loss/leakage, battery life, etc.
Going paperless - in summary
Going paperless is a great goal for many behavioral health programs. However, not all digital systems are created equal. We have conversations with programs around the country who have gone to great lengths to adopt their EHR’s Q15 module, only to revert back to paper because the EHR was more difficult than their paper checks. Similarly, we have spoken with companies who adopted new digital rounding platforms and had to terminate contracts after realizing that ongoing equipment expenses far exceeded their budgeting expectations. Long-term lock-in contracts make these issues even more painful and costly, because the hidden costs and complexities often take time to discover.
The VisibleHand Approach
First off, please do not hesitate to contact us if you have any questions as you consider digital safety check options. Whether you’re considering an EHR module, a security solution, or a digital rounding product like VisibleHand, we’re happy to consult with your team on common pitfalls - from equipment management, to data and analytics, and app functionality.
If you do consider VisibleHand for digital rounding/Q15/safety checks, know that we invest heavily into all three pillars of successful digital rounding adoption.
- We created a simple app that can be launched after just a couple Zoom training sessions.
- We developed reports and analytics that improve transparency and reduce workload for your management team.
- We take care of ALL equipment-related infrastructure and logistics on your behalf, with our *month-to-month, no lock-in *subscription that includes cellular data and free proximity equipment replacement.
